E-stim Summary:
- Electrical stimulation (e-stim) can be used for restoring muscle function following injury and surgery. It can also be used for pain management in reducing perceived discomfort for restoration of movement and function.
- Electrical stimulation is administered through a variety of parameters that are based on targeted response, patient tolerance and goals.
- Over the years electrical stimulation has moved away from solo application and used more in conjunction with movement-based approaches. Pain management combined with exercise-based routines has been shown to produce greater outcomes for restoration of function.
- Electrical stimulation is a form of a non-medicinal modality but patient tolerance and adaptation to the-stimulus can occur. Regardless, it is a safe, affordable and easy to use option compared to more dangerous and risky options such as opioids. Opioids have their place but options like electrical stimulation have less risk of dependency and side effects.
- The best e-stim unit for in home use is the iReliev Wireless TENS + EMS Muscle Stimulator
What Is E-stim?
Electrical stimulation is a modality that has been used in the rehab setting for decades. It is one of the most popular forms of treatments implemented by physical therapists, chiropractors and physicians.
Patients will often inquire as to what electrical stimulation is and if it has any benefit towards improving their recovery process. There has been a lot of research conducted using electrical stimulation to better understand its use, effectiveness and long-term outcomes.
Electrical stimulation used to be a go-to treatment that was almost always used in therapy clinics alongside other modalities such as ultrasound, heat and ice.
In recent years, research and clinical outcomes have provided a better understanding of the most appropriate use of electrical stimulation in order to improve treatment quality and effectiveness.
In this article we will discuss what electrical stimulation is, how it is used and where it has its place currently in the rehab and sports performance setting.
What Injuries Is It Commonly Used On?
E-stim may be appropriate for the following injuries or conditions:
- Back Pain
- Joint Pain
- Muscle Injuries
- Nerve Inflammation
- Arthritis
Always check with your healthcare provider before doing self-treatment with e-stim.
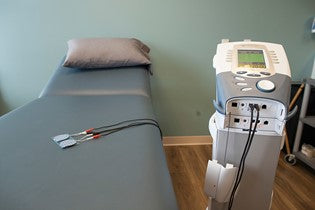
How Does E-stim Work?
Electrical stimulation is basically a microform of electrical currents used to generate muscle contractions for the purpose of restoring strength and muscle function.
It also can be used for pain management by administering it in waveforms that help to send a message to the central nervous system to reduce the sensation of pain.
What Are The Main Types Of E-stim?
Neuromuscular Electrical Stimulation (NMES),Transcutaneous Electrical Nerve-stimulation (TENS) and Functional Electrical Stimulation (FES) are the common forms of administration.
- NMES is for muscle function
- FES is for the muscle function during activity
- TENS is for pain although there can be some variables in the use of these forms.
- Iontophoresis is another form used to help drive medication trans dermally to a localized area.

Russian NMES
“Russian” is a highly concentrated form of NMES which is applied for muscle recruitment. It received its name from Russian scientists experimenting with athletes in the 1960s using the electrical stimulation on their muscles while performing exercises, specifically weight lifting.
The goal was to see if using the-stimulation alongside exercise could make strength improvements.
Some quick science:
TENS activates large diameter afferent fibers, which results in input sent to the central nervous system to activate descending inhibitory systems to reduce hyperalgesia.
Higher intensities of TENS produce B endorphins in the bloodstream and cerebrospinal fluid. Opioid GABA and muscarinic receptors are also activated through TENS but some individuals cannot tolerate high intensity of TENS.
The key point: In other words, the sensation of the electrical stimulation sends a different message to your brain to perceive the feeling of the electrical stimulation instead of the input from the pain. Higher intensities are better if tolerable.
NMES works a little simpler than the pain science methods behind TENS. Through adjustment of wavelengths and intensity, muscle fiber types are targeted producing a contraction.
The higher the intensity is not always better as this can be very uncomfortable for the individual.
Varying the parameters can help allow for muscle contraction while minimizing levels of discomfort. The contraction is localized and involuntary but if the person contracts the muscle along with the-stimulation, it can help to reduce the discomfort.
How To E-stim
Most often the treatment is administered through pads that attach to the skin. The skin contact side of the pad has a sticky gel, which helps the pad adhere to the skin surface.
The pads are applied at the muscle belly or the thickest part of the muscle, sometimes referred to as the acupoint locations, which is the same region needles are applied during acupuncture treatment.
How To Get The Pads Sticky
If you have your own e stim machine at home, you may notice that the pads become less sticky and won’t stay on your skin. To solve this problem, wipe a damp cloth over the pads.
Additionally, you can run a toothbrush over the pads to expose more of the sticky surface so they adhere better.
E-stim For Pain Management
For pain management, the pads are usually applied over the region where pain is being experienced as well as muscle belly locations, depending on the source of pain.
Sometimes pain is referring from a muscle or nerve and sometimes it is from a direct tissue trauma.

The treatment is administered through variables such as time, dosage, ramp sup speed, wavelength, and intensity. Generally the parameters are set to patient tolerance.
For example, NMES or Russian has a more concentrated wavelength with high intensity where it will actually cause the muscle to contract. Sometimes the contraction is too intense for some individuals as described earlier but actively contracting the muscles can help to decrease the sensitivity.
The-stimulation feels like thousands of pins and needles poking into the skin at once, similar to when your hand or foot “falls asleep”.
TENS is applied similarly except the waveforms are different in that they generally do not need to cause muscle contractions. The sensation of the “tingling” is felt instead of the pain.
Sometimes small contractions and quivers of the muscle can help with the pain.
An example of how NMES would be applied would be:
- 10 minutes, 10/30, 32Mhz, ramp up time 2 seconds, Russian. This is a parameter for quad contraction used to help restore quad function following ACL or knee replacement surgery.
- Total time is 10 minutes, the ON for 10 seconds, OFF for 30 seconds, 2 seconds to reach max intensity, intensity is 32 Mhz and the form is Russian meaning the wave length will cause the contraction of the muscle.
- The Mhz is increased to a setting sufficient enough to cause the muscle to contract but also to the patient tolerance.
- Increasing the intensity of Mhz too high can be uncomfortable and noxious to the individual but as they tolerate it more, generally the Mhz can be increased for a more powerful contraction.

The administrations of the-stimulation can an adjusted in forms of pulsing, alternating and non-uniform wavelengths.
This is mostly applied more for pain management with TENS so the individual does not become accustom to the-stimulation as after a period of time, individuals develop a tolerance to the-stimulation, reducing its effectiveness. This is an important consideration for chronic pain patients.

Example of wavelengths demonstrating the variety of delivery of electrical stimulation.
Research On E-stim
If you want to really dive into the science behind the differences of electrical stimulation currents you can find information from sources directly describing electrical stimulation and modalities but unless you are a clinician conducting research, those fine details are not essential towards understanding the purpose of electrical stimulation.
The main take home components are muscle activation, pain management and restoration of function. The parameters are adjusted based on patient tolerance, response of muscle activation, pain relief and also execution of movement.
If you experience an injury and require rehab, the information here will hopefully help you understand why your healthcare practitioner may choose to use or not to use electrical stimulation as part of your treatment plan.
As stated before, electrical stimulation was once a standard form of treatment for a majority of injuries but as we progress through time with a better understanding of human performance and function, research has started to investigate the true efficacy of electrical stimulation and where its use is most beneficial.
Muscle Strength
Currently, electrical stimulation is still being used for muscle strength purposes in the form of NMES.
Most commonly used for quad activation, especially the vastus medialis (VMO) which is greatly affected following ACL surgery, total knee replacement, patella femoral pain syndrome and any invasive joint surgery such as cartilage repair procedures.
Inactivity and shut down of the muscles from bracing and immobilization as well as swelling are all factors following surgery that can affect the quad function so NMES has been shown to be very beneficial towards restoring quadriceps function.
If a person cannot contract their thigh muscles after a surgery, NMES is definitely indicated but even if they can contract the muscles themselves, use of NMES has been shown to help improve the muscle strength and knee extensor strength at a greater rate.

Muscle Function
NMES is also beneficial in restoring muscle function following shoulder dislocation from trauma or even a stroke.
It can also be used to help muscle function following rotator cuff repair when used with caution and monitored parameters so as not to disrupt the repaired tissue.
Use of FES can used for conditions such as foot drop following a traumatic injury or nerve damage resulting from diabetes, herniated discs or fractures. The-stimulation is applied to contract the muscle for function during walking to help the person elevate the foot for clearance off the ground.
This can be used as a rehabilitation solution or if there is permanent nerve/muscle function damage, a lifetime solution can be applied that comes in a form of a custom fitted brace outfitted with stimulation units.

On the left: Use of electrodes on the peroneals and tibialis anterior to help facilitate dorsiflexion following a foot drop injury. Below: Use of a functional electrical stimulation unit to help for dorsiflexion during everyday activity such as walking.


Use of electrodes on the suprasprinatus and posterior deltoid muscles for shoulder dislocation, restoring joint approximation by helping to elevate and retract the head of the humerus back towards the center of the joint.
Pain Management
For pain management, TENS is still used as a non-medicinal modality. TENS use is a safe, affordable, self management tool that can be used in helping individuals return to a normal level of function.
TENS can be administered in the portable units as described earlier or in braces such as the one below fitted for the low back. This option is something an individual can use while working.

With that previous statement, caution needs to be implemented.
The act of simply blocking ones pain can be dangerous towards disposing the person for further injury.
As electrical stimulation offers a form of non-medicinal pain management and falls under the same scope of management through oral medications in the sense of the underlying issue still needs to be corrected.
If there is true mechanical dysfunction, instability and strength deficits, the pain is a message that the body is not functioning properly and just blocking the pain through medications or stimulation is not the proper solution.
Research and clinical outcomes have demonstrated that use of electrical stimulation alone is not efficient enough towards reducing pain and restoring function but rather movement and exercise based programs in conjunction with pain management methods such as electrical stimulation is most beneficial.
The pain management resources should be used to help facilitate movement-based approaches.

Simply put, if your back hurts because the muscles are excessively tight and guarding due to compensation, slapping some electrical stimulation on it is not the solution.
Using the-stimulation to help reduce pain so you can restore normal tissue properties in the lumbar muscles and improve proper function of the appropriate muscles required for torso stabilization is a more appropriate option.
For chronic pain patients, TENS has its place but due to daily use, the parameters will have to be adjusted so that the individual does not adapt to it and create a tolerance to the-stimulus.
Studies have shown that the use of TENS can help manage pain, allowing for restoration of movement and function but the challenge is to help the person engage in activity and movement without reliance on the TENS unit.
With the rising use and research involving other forms of pain management techniques such as CBD oil, the convenience and positive outcome rates may surpass those of electrical stimulation.
E-stim For Muscle Growth And Strength
There have been studies investigating use of the products such as stimulation belts for the abdominals. Studies have demonstrated improvement in muscle function as in accordance with rehab studies but remember that electrical stimulation is primarily an involuntary contraction of the muscles.
The-stimulation unit is doing the work as opposed to the message being sent from the brain to the muscle. If one was to exercise and complete movements with the-stimulation pads on such as what the Russians were doing in the 1960s, that would be a different form of application.
Still there is not enough conclusive research or outcomes to demonstrate that the combination of electrical stimulation with exercise is better than exercise alone.
E-stim Risks
While using e-stim is very safe for most individuals there are a few things that could cause pain and other conditions where a person should not use s-stim:
- If the e-stim is set to high it can cause a powerful muscle contraction that could lead to injury.
- The e-stim pads can sometimes cause skin irritation on sensitive individuals.
- Anyone with a pacemaker should NEVER use e-stim.
- Women who are pregnant should consult a healthcare professional before using e-stim.
About The Author:
Michael St. George PT, DPT has been practicing for 10 years primarily in the outpatient and orthopedic setting. He works for a physical therapist owned private practice based in the greater Philadelphia area and surrounding suburbs. Mike is certified through Functional Movement Systems for FMS, SFMA and FCS which consist of screens and testing used to measure movement quality and performance. Mike also has experience with working with numerous surgeons and physicians from the Rothman institute. Currently he works primarily with ACL, meniscus and post surgical recovery and sports injuries, return to sport testing and performance, running evaluation and re training and hand and upper extremity conditions.
References:
- Hollis, S., Mcclure, P. (2017) Intramuscular Electrical Stimulation for Muscle Activation of the Tibilias Anterior After Surgical Repair: A Case Report. Journal of Orthopaedic and Sports Physical Therapy. Vol 47 (12) 965-969
- Adams, C., Wayne, S., Basile, J., et al. Electrically Elicitied Quadriceps Muscle Torque: A Comparison of 3 Waveforms. (2018) Journal of Orthopaedic and Sports Physical Therapy. Vol 48 (3) 217-224
- GTVance, C., Dailey, D., Rakel, B. et al. Using TENS for pain control: the state of the evidence. (2014) Pain Management. Vol 4 (3) 197-209
- Liebano, R., Waszczuk, S., Correa, J. (2013) The Effect of Burst-Duty-Cycle Parameters of Medium-Frequency Alternating Current on Maximally Electrically Induced Torque of the Quadriceps Femoris, Discomfort, And Tolerated Current Amplitude in Professional Soccer Players. Journal of Orthopaedic and Sports Physical Therapy. Vol 43 (12) 920-926.
- Kim, K., Croy, T., Hertel, J. Saliba, S. (2010) Effects of Neuromuscular Electrical Stimulation After Anterior Cruciate Ligament Reconstruction on Quadriceps Strength, Function, and Patient-Oriented Outcomes: A Systematic Review. Journal of Orthopaedic and Sports Physical Therapy. Vol 40 (7) 383-391
- Louw, A., Sluka, K., Nijs, J. Revisiting the provision of Pain Neuroscience Education: An adjunct intervention for patients, but a primary focus on clinician education.
- Nussbaum, E., Houghton, P., Anthony, J. et al. (2017) Neuromuscular Electrical Stimulation for Treatment of Muscle Impairment: Critical Review and Recommendations for Clinical Practice. Physiotherapy Canada. Vol 69 1-76


